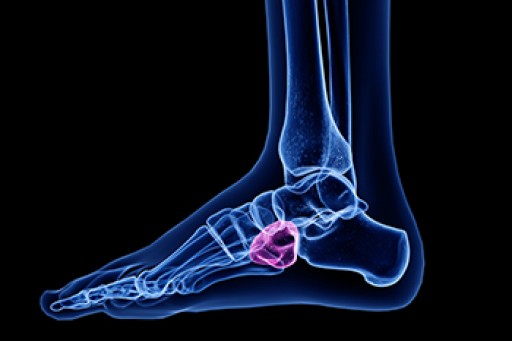
There is a bone in the foot known as the cuboid bone. An injury may cause this bone to shift out of alignment, possibly causing cuboid syndrome to develop. The pain is generally felt on the outer edge of the foot and can be a common injury among dancers and athletes. Usual symptoms that are often experienced with cuboid syndrome can include difficulty in bearing weight on the foot, a reduced range of motion, and the foot may be swollen. Additionally, the pain may begin as a dull ache and gradually sharpen, increasing discomfort on the overall foot. People with flat feet may experience this condition, or it may come from those who frequently engage in running and jumping activities. Mild relief may be found when the affected foot is elevated and the activity that caused the injury is temporarily stopped. If you have pain in this part of your foot, it is suggested that you confer with a podiatrist who can effectively diagnose and treat cuboid syndrome.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with Scott Samera, DPM from Samera / Foot + Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact our office located in Lake City and Branford, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.